Breast Unit
Care after treatment
Care after breast cancer treatment
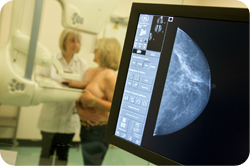
There are usually no routine clinic appointments following breast cancer treatment, unless the surgery has involved a bilateral mastectomy.
However, all patients who have remaining breast tissue will have mammograms at the RUH at years 1, 2, 3, 4, 5, and for patients over the age of 50, further mammograms at year 7 and 9 following treatment. For those still less than 50 years of age, mammograms will continue every year until the age of 50.
During the period following breast cancer diagnosis when mammograms are being done at the RUH, all breast cancer patients should decline any requests for routine screening that are made by the Avon breast screening service or the Wiltshire breast screening service.
Following their final mammogram at the RUH patients can return to the national screening programme.
You will be invited to a "moving on day" following your treatment where a series of talks are given to a group of women who have had breast cancer which will address many of the on going issues faced by our patients.
Telephone support
Also as part of our follow up for all women who have had breast cancer, we offer an open access to our patients to support, diagnose and treat any problems related to their breast cancer. We encourage patients to telephone our breast care nurses who may be able to answer any queries over the telephone or will make an appointment to see a breast surgeon in the next available clinic.
Telephone calls typically concern:
- Problems relating to side effects following treatment, which include:
- Lymphoedema
- Radiotherapy changes
- Side effects of endocrine treatments
- Menopausal symptoms
- Sex and fertility issues
- Depression and emotional support following breast cancer treatment
- Family history
- Cosmetic and breast reconstructive queries
- Problems relating to concerns about breast cancer returning
Will it come back? Has it come back?
Risk of recurrence
Following treatment for breast cancer, many women will be cured. However for some women, breast cancer cells can return either locally (in the breast, where the breast was or in the armpit) or in another part of the body (distant recurrence).
The signs and symptoms of recurrent breast cancer vary depending on where the cancer comes back.
Local recurrence
In a local recurrence, cancer reappears in the same area as your original, or "primary," tumour Signs and symptoms of local recurrence within the same breast may include:- A new lump in your breast or irregular area of firmness
- A new thickening in your breast area
- A new pulling back of the skin or dimpling at the lumpectomy site
- Skin inflammation or area of redness
- Flattening or indentation of your nipple or other nipple changes
Follow up mammograms are in place to pick up local recurrence after breast conserving surgery however mammograms are not 100% accurate and our patients are recommended to look for signs of local recurrence.
Signs and symptoms of local recurrence on the chest wall after a mastectomy may include:
- One or more painless nodules on or under the skin of your chest wall
- A new area of thickening along or near the mastectomy scar
Regional recurrence
A regional breast cancer recurrence means the cancer has come back in the lymph nodes in your armpit or collarbone area. Signs and symptoms of regional recurrence may include:- A lump or swelling in the lymph nodes under your arm or in the groove above your collarbone
- Swelling of your arm
- Persistent pain in your arm and shoulder
- Increasing loss of sensation in your arm and hand
Distant (metastatic) recurrence
A distant, or metastatic, recurrence means the cancer has travelled to distant parts of the body, most commonly the bones, liver and lungs. The signs and symptoms may include:- Pain, such as chest or bone pain
- Persistent, dry cough
- Difficulty breathing
- Loss of appetite
- Persistent nausea, vomiting or weight loss
- Swollen abdomen
- Severe headaches
For women who experience these signs or symptoms, we would encourage them to telephone our breast care nurses.
What can be done to reduce the risk of cancer returning?
The list below has been shown to reduce the risk of breast cancer returning:
- Compliance with antioestrogen medications: For patients with a breast cancer that is sensitive to oestrogen, Tamoxifen or an aromatse inhibitor will have been prescribed for at least 5 years. While this is usually well tolerated, some patients will have side effects. It is important that these tablets are taken for 5 years to reduce the risk of breast cancer returning. We would encourage our patients to come back to clinic if they are having difficulty with their medication.
- Physical activity: Several studies of different types of cancer have suggested that high levels of physical activity can help to lower the risk of cancer recurrence. The exercise was the equivalent of 30 minutes brisk walking four days a week.
- Maintain a healthy weight: After the menopause, your oestrogen levels are linked to the amount of body fat you have. The more body fat you have, the higher your oestrogen levels are likely to be.
- Sensible drinking: Two large combined reviews of the published evidence and the UK Million Women Study showed an increase in risk of about 7 to 12% with every extra unit of alcohol per day. One unit is a half pint of beer, a small glass of wine, or a measure of spirits. To be on the safe side, it is best for women not to drink more than 14 units of alcohol per week.

