Children's Allergy Clinic
Information about allergies
Information about allergies
On this page:Food Allergy
Food allergy is an allergic response to a specific food, where allergic symptoms occur, every time skin contact or ingestion with the food occurs, and is reproducible.
The main treatment for food allergy is avoidance of the allergen responsible, and for some, access to medication to reduce symptoms if they occur.
This can occur in two ways:
IgE mediated
Symptoms occur immediately, or within one hour of contact with a specific food, and occurs each time there is contact with the same food. Symptoms can include; hives (urticaria), itching, vomiting, swelling (Angioedema), wheeze or collapse.
Any food can cause this type of allergic condition, and skin prick testing or Specific IgE blood tests can be performed to establish true cause and ongoing treatment regimes.
Non-IgE mediated
Symptoms usually occur much later after contact with a food, from 2-24 hours contact with a food. This type of response predominantly occurs with milk and soya, but can occasionally occur for some with egg and wheat. Symptoms are often gut or skin related, with eczema, diarrhoea, constipation, apparent abdominal discomfort, and reflux being the most common symptoms.
There are no tests for this type of allergy - the testing is to remove the possible food, one food at a time for 2-3 weeks, and then reintroduce a small amount of the food gradually to establish true cause.
If an improvement is seen:
- remove that food from the diet, if no improvement is seen then the cause is not that food
- introduce the food back into the diet, and seek support from your GP about what to do next
- you may need advice from a dietitian to replace essential nutrients.
Food challenge
The gold standard test as to whether someone has an IgE food allergy is:
"
Can they eat a food without allergic symptoms occurring?"
If testing suggests you have outgrown an allergy, or the cause of your problem may not be allergic in nature, we may suggest a food challenge.
This involves you either reintroducing the food at home following a cautious plan discussed with the team, or attending an appointment at a later date to re-introduce the food in a clinic environment - your clinical history dictates which type of challenge is most suitable.
We would NOT advocate trying a food before you have been reviewed by one of the team.
Food challenge information
Food Challenge Consent Form (download to complete)
RUH Allergy Food Ladders
Allergy support:
01322 619898
Asthma
Asthma is a condition of the airways, which may not be linked to allergy, however, does commonly affect those with other allergic conditions. It is a serious condition that should be managed with support from your GP or specialist asthma nurse.
If a regular steroid inhaler is prescribed, it should not be stopped without discussion with your healthcare professional. The reliever inhaler should be kept close to hand. If you are using your reliever inhaler frequently (more than 3 times a week, when you are generally well), you should have an asthma review.
You can find more information to support you here:
RUH Paediatrics information about Asthma
How to use an inhaler (Asthma UK)
Are you at risk of an asthma attack? - Asthma UK Online asthma symptom checker
Hay fever & Asthma leaflet (Allergy UK)
Allergic Rhinitis (Hay Fever)
Seasonal Allergic Rhinitis also known as hay fever, can be debilitating and hard to live with. For those who are severely affected, it can significantly affect mood, sleep and impact their behaviour. It can occur for just a month or so or can be yearlong if involving more than one type of pollen (e.g. trees and grass).
Rhinitis can also occur throughout the rest of the year due to other allergens such as house Dust Mite.
Allergy testing is not always needed but may sometimes be recommended in very severe cases not improving with regular treatment.
Symptoms can vary year to year, and can range from a stuffy, congested to nose, to a permanent runny nose, along with itchy, dry eyes, and repeated bouts of sneezing.
As management of allergies is generally through avoidance, this type of allergy can be very challenging, and the main treatment for environmental allergies is management of symptoms, through use of antihistamine and various nasal or eye treatments. The treatments available depend on the severity of symptoms, and age of the child.
Allergic Rhinitis & Hay fever factsheet (Allergy UK)
Asthma & Hay Fever (Asthma UK)
How to use your Nasal Spray (Allergy UK)
Allergic Eye Disease Factsheet (Allergy UK)
Hay Fever & Asthma leaflet (Allergy UK)
Allergy Hay Fever Support
Tel: 01322 619898
Pollen Level Apps are available here:
|
|
klarify: Pollen allergy tracker |
|
|
My Pollen Forecast |
Immunotherapy
Immunotherapy is an oral treatment regime over a 3-year period for those with unmanageable seasonal allergic rhinitis (hay fever). To access this service the allergic individual must be having severe symptoms despite maximum treatment with antihistamines, eye drops and nasal sprays and still continue to have unmanageable symptoms.
If you think this applies, ask your child's GP for a referral to the allergy team for assessment for this programme. There are currently limited resources for immunotherapy so only those who meet the criteria as above can be considered. We may ask you and your child to go away and increase treatments before your child can be considered for the programme.
Allergy UK Immunotherapy Factsheet
Anaphylaxis
Anaphylaxis is the more severe form of allergic reaction, including more serious symptoms such as difficulty breathing or loss of consciousness.
If we consider that there is a risk of anaphylaxis we will discuss this with you and may prescribe an Adrenaline Auto-Injector (AAI), commonly known as EpiPen, Jext, or Emerade. It is not necessary for everyone with a food allergy to require an AAI.
We assess the risk of anaphylaxis at every appointment, and it is dependent on a number of clinical factors which will be discussed at every review.
These websites contain information about AAI's, how to use them, expiry alert services and resources for children and young people. There are video's on each site which can be helpful to share with wider family or friends.
Eczema and rashes
Eczema is a common skin condition which commonly affects those with other allergic conditions, it can be the precursor to allergy - as uncontrolled eczema can cause an infant to develop allergies through contact with their damaged skin.
If your baby has eczema - see the GP, and use the treatments provided as prescribed, applying the moisturiser (Emollients), as frequently as possible. Steroid creams may also be needed and are very effective and safe.
Some can foods can irritate the sensitive skin of under 1's, or cause an exacerbation of eczema. This is common with acidic foods, such as tomato, fruits, or food with rough textures, such as toast, or crackers. Generally if the rash doesn't appear to bother the child, then it is unlikely to be allergic in nature. Allergic rashes are usually intensely itchy and significantly distress the child.
Rashes can also occur in young children during a viral illness - if a rash continues despite giving antihistamine, then the cause is less likely to be allergic in nature.
Sometimes hives type rashes (urticaria, nettle rash) and skin swelling can occur without any obvious cause. Regular non-drowsy antihistamines such as cetirizine can be helpful, if this continues then it should be investigated.
More information on rashes can be found here:
National Eczema Society Helpline
Tel: 0800 448 0818
Chronic Spontaneous Urticaria & Angioedema
Chronic Spontaneous Urticaria & Angioedema is a condition that involves rashes or swelling with an unknown trigger. It is a condition that can be incredibly debilitating, difficult to manage and often has distressing symptoms. It can significantly affect mental health, sleep, and school attendance.
Rash symptoms can vary from mild hives, type rashes on small areas of the body, to whole body itchy, uncomfortable hives that cause significant anxiety for the person involved.
Swelling can occur for some, this may be lips, or eyes and can vary from person to person in its intensity. It can also be very distressing and quite frightening for the sufferer and anyone else observing the sufferer.
Unfortunately there is no specific testing for this condition, although blood test can be done if the condition persists, and there is still little known about the likely triggers. There is also very little known about duration of incidence – for some it will be an occasional occurrence, and never appear again. However some suffer for a number of years with it. It can in some cases come and go over several years.
Urticaria & Angioedema leaflet (Allergy UK)
What is Chronic Spontaneous Urticaria? (Allergy UK info & video)
Chronic Spontaneous Urticaria (CSU): Does it rule your life? (Allergy UK)
Chronic Spontaneous Urticaria Images:
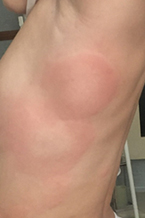 |
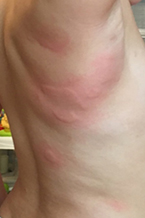 |
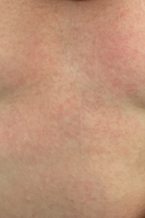 |
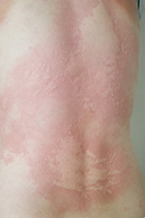 |
Under 5's allergy resources and support
Weaning for the allergic infant
The evidence shows that it is important for babies with a known milk allergy, eczema or a family history of allergy to introduce allergic-type foods - e.g. peanut and egg as early as possible once a baby starts having solid foods. The ideal would be starting egg and peanut butter from 4-6 months of age, alongside breastfeeds/alternative milks.
It is important for a child who has developed allergies already that the other allergens are introduced into the child's diet. This can prevent them from developing an allergy to another food in the future. Parental allergy is not an indicator of a child developing the same kind of allergy.
Guidance below may help with this, as well as having some antihistamine to hand before trying other allergens:
School age allergy resources and support
Anaphylaxis Training for Early Years Settings & School Allergy information
School Nurses across Wiltshire and BaNES provide support and can signpost to free training for all LEA schools.
Any setting can access this free training, and every child who attends the RUH allergy clinic will be supplied with an Action Plan for use in EYS or school, the team are happy to support settings via their HCP dedicated email address: ruh-tr.paediatricallergy@nhs.net
Allergy Advice
5-11 years
Auto-Injector advice 7-11 years
Useful books for teaching children about allergy age 3-8 years:- Freddy the mouse
- The Allergic Princess
Teens
Food allergy alert services
Becoming independent with allergies
Adrenaline Auto-Injector Information & Resources
EpiPen

