Breast Unit
Sentinel Lymph Node Biopsy
Sentinel Lymph Node Biopsy
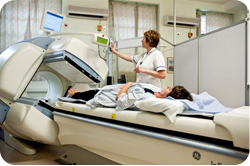 Preparing the patient for sentinel node imaging |
On this page: What is it? Why is it done? How is it done? How reliable is the technique? What are the possible complications? What happens next? Travelling after your procedure |
What is a Sentinel Lymph Node Biopsy
Sentinel lymph node biopsy is the surgical removal of one or more small lymph glands from the axilla (armpit) that lies close to the breast.
Why is it done?
When treating patients for breast cancer it is important to know whether the cancer has spread outside of the breast. This has a strong bearing on how the cancer is behaving and what treatments may be required in addition to surgery.
At present the best method to detect such spread is to analyse some of the lymph nodes in the armpit because this area is often the first place affected outside of the breast.
The most reliable way to find this out is to actually remove some of these lymph nodes at an operation. Unfortunately, there are no simple tests that can reliably give us this information, without actually doing an operation.
It is thought that the sentinel lymph node (SLN) is the pivotal node that drains the breast and the tumour. If the breast cancer has spread it is most likely to have spread to this node first.
How is it done?
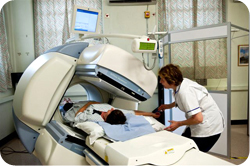
Patient being scanned by the gamma camera during sentinel node imaging
The SLN is removed during the main operation to excise the breast cancer but additional scans in the Nuclear Medicine Department are done before this to locate its position.
During this imaging procedure a small amount of a radioactive tracer will be injected in the skin of the breast by a specially trained technician. This tracer travels through the breast tissue and is taken up in the SLN.
Soon after the injection images will be taken using a special detector which will be placed close to the side of your breast. Two images are usually acquired each taking 1 minute. The speed at which the tracer flows into the SLN cannot be anticipated so you may be in the department from anywhere between 30 minutes to 2 or 3 hours.
The Department of Nuclear Medicine is located in RUH South. You may want someone to come with you on the day of the scan – this is fine. However we have only one waiting room so we advise you not to be accompanied by children or pregnant women (this helps to minimise radiation exposure to these people).
If you have any concerns or questions with regard to the SLN Imaging procedure you can telephone the Nuclear Medicine Department on 01225 824080.
The radioactive tracer injection and imaging procedure should not make you feel any different. The radioactive tracer injection does sting a little while being administered but this feeling will quickly subside.
The radioactive substance is used as sparingly as possible. The dose is very low, similar to the natural background radiation that you receive in a year. It is quickly eliminated from your body.
The radiation dose to other people around you on the day of your scan is low and is not a cause for concern. However, there is a very small risk to an unborn or breast-feeding child. So, it is important that you let us know in advance if you are breastfeeding or if there is a chance that you might be pregnant.
The operation itself is performed either later the same day or the following day. During this operation a blue dye is also injected into the breast. Then the surgeon will look for and remove the SLN which should be blue and slightly radioactive as detected using a gamma probe in the operating theatre during the operation.
How reliable is this technique?
This is an accurate and reliable test but it is important to understand that it is NOT absolutely 100% accurate. In about 1 out of 10 cases the surgeon may not be able to find the SLN, in which case it may be necessary to perform an axillary dissection whereby the majority of the lymph nodes in the lower armpit are removed.
Also, there is a small chance that test could give a falsely reassuring result (in less than 1 out of 10 cases). To try and reduce this chance of error we frequently try to remove more than one lymph node at the time of the procedure.
What are the possible complications?
Most patients would not develop problems and complications from this part of the operation. However, obviously the area will be sore and uncomfortable immediately afterwards, it may be swollen and your shoulder movements will be reduced somewhat.
The discomfort should improve rapidly as the days pass and shoulder movements should return to normal.
Some patients may develop other problems, such as a wound infection, post-operative bleeding or the development of a fluid collection in the wound itself (a seroma). These are not major problems and should be readily treatable.
A seroma might need to be drained with a needle in the outpatient clinic afterwards. There is a very small risk that arm or hand may become swollen and enlarged afterwards, a condition called lymphoedema.
Lymphoedema - Causes and Prevention
Link opens in a new window
The blue dye used for the test does have a number of possible side effects. It will discolour the skin of the breast where the injection was placed. This discolouration may persist for many months and indeed it may be permanent in some women. The dye makes people turn grey in colour and their urine turns green. This discolouration may persist for a few days.
Lastly, a small number of people are allergic to the dye. Minor allergic reactions are seen in just 2 out of every 100 patients. Major allergic reactions (anaphylaxis) are seen in 1 every 500 patients.
What happens next?
After the operation has finished the SLN is analysed by a pathologist to find out what is happening at a microscopic level. Obviously, we hope that no cancer cells are seen.
However, it is very important for you to understand that if tumour cells were found to be present in the SLN a second operation might be required at a later date to remove the remaining lymph nodes in the armpit as there is a strong chance that these nodes could harbour cancer cells within them as well.
Travelling after your procedure
Some airports, seaports and train stations around the world have installed very sensitive radiation detectors.
On the days following any Nuclear Medicine procedure, it is possible that these detectors may be triggered by the small amount of radioactivity remaining in your body. Therefore, if you are planning to travel within the 7 days following your procedure, it is recommended that you carry your appointment letter and this information leaflet to show to customs officials if necessary.
Also See:
Wide Local Excision (Lumpectomy)
Needle Localised wide local excision
Axillary Lymph Node Dissection
Mastectomy without reconstruction

